
Every year, about 250,000 people in the U.S. with severe obesity and related health conditions undergo bariatric surgeries. These procedures can help people lose excess weight and rapidly improve high blood sugar, high blood pressure and heart disease.
Some of these changes result from restricting the amount of food the stomach can hold. Others arise from post-surgical changes in hormone levels and other aspects of metabolism that researchers are still trying to fully grasp.
A new study from Harvard Medical School and Brigham and Women's Hospital reveals the latest piece of the puzzle of how bariatric surgery can lead to healthier blood sugar levels.
The researchers report in Nature Chemical Biology that a specific bile acid—a component of bile produced in the liver—rises in the guts of mice and humans after bariatric surgery and sets off a chain of biochemical events that lowers high blood sugar.
The findings point to a potential new drug candidate for treating disorders of blood sugar regulation, such as type 2 diabetes.
"These findings are exciting because, to our knowledge, it’s the first time someone has identified an anti-diabetic small molecule whose levels are increased by bariatric surgery," said A. Sloan Devlin, assistant professor of biological chemistry and molecular pharmacology in the Blavatnik Institute at HMS.
Devlin is co-senior author of the study with Eric Sheu, HMS assistant professor of surgery at Brigham and Women's.
"It's exciting to find that this bile acid, previously believed to be a waste product, has glucose-regulating effects in mice," said Sheu. "It will be important to further explore our findings to determine whether it can be turned into a drug that helps patients as well."
Acid test
The team analyzed intestinal samples from mice and stool samples from people before and after sleeve gastrectomy, one of the most common bariatric surgeries, in which surgeons remove about 80 percent of the stomach.
The researchers focused on bile acids in the gut. These acids help us digest fats and vitamins and convey signals that help regulate metabolic and immune functions. Scientists are still uncovering bile acids' roles as communication agents in the body.
Previous studies had indicated that bile acids as a group rise in the bloodstream after bariatric surgery, but to date, no one had studied the effects of surgery on individual bile acids nor on bile acids in the gut alone, where a key blood sugar-regulating hormone known as GLP-1 is made.
GLP-1 also rises after bariatric surgery. Clinicians suspect that this is one of the ways the surgery improves type 2 diabetes.
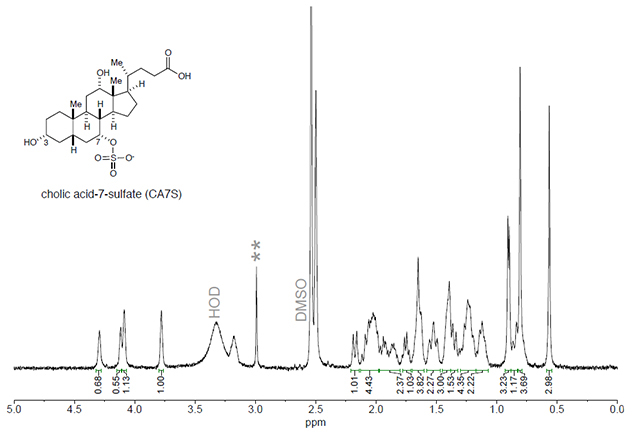
When Devlin and Sheu's teams conducted their analyses, one bile acid—cholic acid 7-sulfate, or CA7S—jumped out. Of more than 50 bile acids, it alone rose significantly after sleeve gastrectomy.
The researchers found that like a few other known bile acids, CA7S activates a receptor called TGR5 on the surface of certain cells in the intestinal lining. TGR5 then spurs the cells to secrete GLP-1, which stimulates the pancreas to secrete insulin, encouraging cells to absorb sugar from the bloodstream after eating.
"Our work helps answer the questions of why and how this anti-diabetic hormone rises after surgery," said Sheu.
To confirm the effects of CA7S, the researchers fed the bile acid to mice with diet-induced insulin resistance, a key feature of type 2 diabetes. After treatment, the mice were more sensitive to insulin, metabolized glucose better and had lower blood sugar levels than mice without the bile acid.
These benefits disappeared when the researchers used genetic tools to prevent the mice from producing TGR5.
Strength in specificity
TGR5 receptors are of increasing interest in the research community as a drug target for improving metabolic health, and there are many ongoing efforts to craft synthetic molecules that activate them<.
Devlin and Sheu’s experiments revealed that CA7S activates TGR5 more efficiently than these synthetic compounds.
Researchers have identified a handful of natural bile acids that activate TGR5. Devlin and Sheu found that CA7S is just as potent.
Their experiments suggest that CA7S has potential as a drug—or the foundation for a drug—to manipulate the receptor and help regulate blood sugar, the authors said.
Although it's not yet clear whether CA7S will prove a safe and effective treatment for type 2 diabetes and other blood sugar-related conditions in humans, it has several potential advantages, the authors said.
First, while other natural and synthetic TGR5 activators spread into the bloodstream and bind to TGR5 receptors in unwanted parts of the body, the researchers found that CA7S stays in the gut. That could reduce side effects, they said.
Second, the team found that CA7S stimulates cells to sprout more TGR5 receptors, allowing other molecules to lock on and join the call to improve blood sugar levels.
"These findings show why it's important to study individual bile acids, as opposed to whole groups of them at once, and to study them locally, in the gut," said Devlin. "These compounds each have their own molecular binding preferences that give them unique abilities to modulate blood sugar, fat metabolism and energy expenditure."
Bile acid production and chemistry can be affected by bacteria in the intestines. Since bariatric surgery also alters the gut microbiome, Devlin and Sheu plan to explore potential interactions between gut bacteria and CA7S next.
The two lab leaders emphasized that their groups wouldn't have made these discoveries about CA7S if they hadn't collaborated.
"Chemists and cell biologists from our lab worked together with surgeons from the Sheu lab to discover this potential new anti-diabetic molecule," said Devlin.
Funding and authorship
Snehal Chaudhari, research fellow in biological chemistry and molecular pharmacology in the Devlin lab, and David A. Harris, HMS clinical fellow in surgery at Brigham and Women's, are co-first authors of the study. Additional authors are Hassan Aliakbarian, James N. Luo, Matthew Henke, Renuka Subramaniam, Ashley Vernon and Ali Tavakkoli.
This study was supported in part by the National Institutes of Health (grants P30DK057521 and R35GM128618), Joslin Diabetes Center (P30DK036836), HMS Department of Biological Chemistry and Molecular Pharmacology, Harvard Catalyst (4KL2TR001100-04), HMS Quadrangle Fund for Advancing and Seeding Translational Research (Q-FASTR) and Blavatnik Biomedical Accelerator at Harvard University.





